A panic attack is a single, time-limited episode of intense fear with physical symptoms including racing heart, breathlessness, chest tightness, and dizziness, typically peaking within ten minutes. Panic disorder is a diagnosable condition defined by recurrent, unexpected panic attacks combined with persistent worry about further attacks or significant behaviour change to avoid them. Not everyone who experiences a panic attack has panic disorder. NICE guideline CG113 recommends CBT as the first-line psychological treatment for panic disorder in the UK, supported by the World Health Organisation. CBT is the right step when panic attacks are recurrent, unexpected, and beginning to shape how you live your life.
Panic Attacks vs Panic Disorder: What Is the Difference and When Is CBT Right for You?
Your heart is hammering. Your hands are shaking. You cannot catch your breath, and somewhere in the back of your mind a voice is telling you something is very wrong. Whether it lasts two minutes or twenty, a panic attack is one of the most physically overwhelming experiences a person can have. And one of the most frightening things about it, once the episode passes, is not knowing what it means.
Was it a one-off? Is it going to happen again? Does having a panic attack mean something is seriously wrong with you, physically or psychologically? And at what point should you actually do something about it?
These are the questions most people are sitting with when they search for answers, often alone, often late at night, often after it has already happened more than once. This article gives you clear, evidence-based answers: what panic attacks are, what panic disorder is, how the two differ, and when CBT is the treatment that is genuinely right for you.
Key Takeaways
- A panic attack is an event, not a diagnosis. Many people experience at least one in their lifetime without ever developing panic disorder (Mind UK).
- Panic disorder is defined by recurrent, unexpected panic attacks combined with at least one month of persistent worry about further attacks or significant behaviour change in response to them (NICE CG113).
- The physical symptoms of a panic attack, including chest pain, racing heart, and breathlessness, are real and produced by the body's genuine alarm response. They are not imagined, exaggerated, or a sign of weakness.
- NICE guideline CG113 recommends CBT as the first-line psychological treatment for panic disorder. Panic disorder is one of the most treatment-responsive anxiety conditions: most people who engage with CBT experience significant improvement.
- CBT is not always necessary after a single panic attack. It becomes the right choice when attacks are recurrent, when anticipatory anxiety develops between them, or when avoidance is beginning to narrow your daily life.
What is a panic attack?
A panic attack is a sudden episode of intense fear or discomfort that peaks within minutes and triggers a range of powerful physical and psychological symptoms. The NHS describes it as an exaggerated response of the body's natural alarm system: the fight-or-flight response activating, often in the complete absence of any actual danger.
Symptoms typically include a racing or pounding heart, chest tightness or pain, shortness of breath, trembling or shaking, sweating, nausea, dizziness, numbness or tingling in the hands or face, and a sense of unreality or detachment from your surroundings. Many people experiencing their first panic attack believe they are having a heart attack or are about to lose consciousness. That is not an overreaction. The physical experience genuinely feels like a medical emergency, and it is one of the most important things to understand: the symptoms are real. They are produced by your body, not your imagination.
For many people, the first panic attack ends in A&E or an urgent GP appointment. The chest pain, the racing heart, the difficulty breathing: these are symptoms that warrant medical attention when you have no idea what you are experiencing. Tests come back clear. An ECG shows nothing wrong with the heart. A doctor tells you it was most likely anxiety. And then, in the hours and days that follow, many people find that explanation genuinely difficult to accept. The experience felt too physical, too severe, too real to be accounted for by anxiety alone. That difficulty accepting the all-clear is not stubbornness or irrationality. For some people, it is the beginning of something worth taking seriously.
Panic attacks can be expected, occurring in response to a specific trigger, such as a situation, place, or object that has become associated with fear. Or they can be unexpected, appearing to come from nowhere, sometimes waking people from sleep with no obvious cause. It is the unexpected type that is most strongly associated with panic disorder.
Crucially, a panic attack is not a diagnosis in itself. It is an event. Experiencing one panic attack, even a severe one, does not mean you have panic disorder. Many people have a single panic attack and never experience another. The question of what it means depends on what happens next.
Mind UK notes that panic attacks are more common than most people realise. Around one in three people will experience a panic attack at some point in their life. Having a panic attack does not mean something is fundamentally wrong with you. It means your nervous system interpreted something as a threat and responded accordingly.
What is panic disorder?
Panic disorder is a diagnosable anxiety condition in which a person experiences recurrent, unexpected panic attacks and develops significant worry or behaviour change in response to them. According to NICE guideline CG113, the defining features are recurrent unexpected panic attacks combined with at least one month of at least one of the following: persistent concern about having further attacks, worry about what the attacks mean (fearing they signal a serious illness or a loss of control), or a significant change in behaviour related to the attacks.
That last point is important. Panic disorder is not only about how often panic attacks occur. It is about the relationship that develops with them. A central feature is anticipatory anxiety: a background level of unease between attacks, scanning the body for signs that another one might be coming. This often leads to avoidance that begins small and expands quietly over time.
Someone with panic disorder might stop drinking coffee because an elevated heart rate feels threatening. They might avoid exercise for the same reason. They might stop taking certain routes, avoid public transport, or choose not to go anywhere that feels difficult to leave quickly. None of these decisions feel like avoidance at the time. They feel like sensible precautions. But each one reinforces the idea that those situations are genuinely dangerous, and that reinforcement is what keeps panic disorder running.
One of the most common patterns seen clinically is repeated medical help-seeking. Multiple GP appointments about heart palpitations. Requests for cardiac investigations. A return to A&E during a particularly severe episode. Each time, the tests come back clear. Each time, a doctor explains that it is most likely anxiety. And each time, that reassurance holds for a while, and then fades. Because the problem is not a lack of information about what panic attacks are. The problem is that when the next attack arrives, the body's alarm system fires with the same intensity, and the catastrophic interpretation returns just as powerfully: something is seriously wrong. No amount of reassurance from a GP, a cardiologist, a partner, or the internet changes what the body does the next time those sensations escalate. This is one of the clearest reasons why CBT, which works directly on the interpretation and the conditioned physical response, is a categorically different intervention from reassurance. And it is why reassurance alone, however well-intentioned, rarely resolves panic disorder.
The Royal College of Psychiatrists estimates that panic disorder affects approximately 1 to 2 per cent of adults in the UK at any one time, making it one of the more common anxiety conditions seen in both primary and specialist care. It can begin at any age but most often develops in early adulthood.
NICE guideline CG113, covering generalised anxiety disorder and panic disorder in adults, classifies panic disorder under a step-care model. Mild presentations may be supported with psychoeducation and self-help resources initially. Moderate to severe presentations, particularly where avoidance is established, warrant direct access to CBT or medication. The World Health Organisation includes panic disorder in its classification of anxiety disorders as a significant source of disability when left untreated (WHO, 2022).
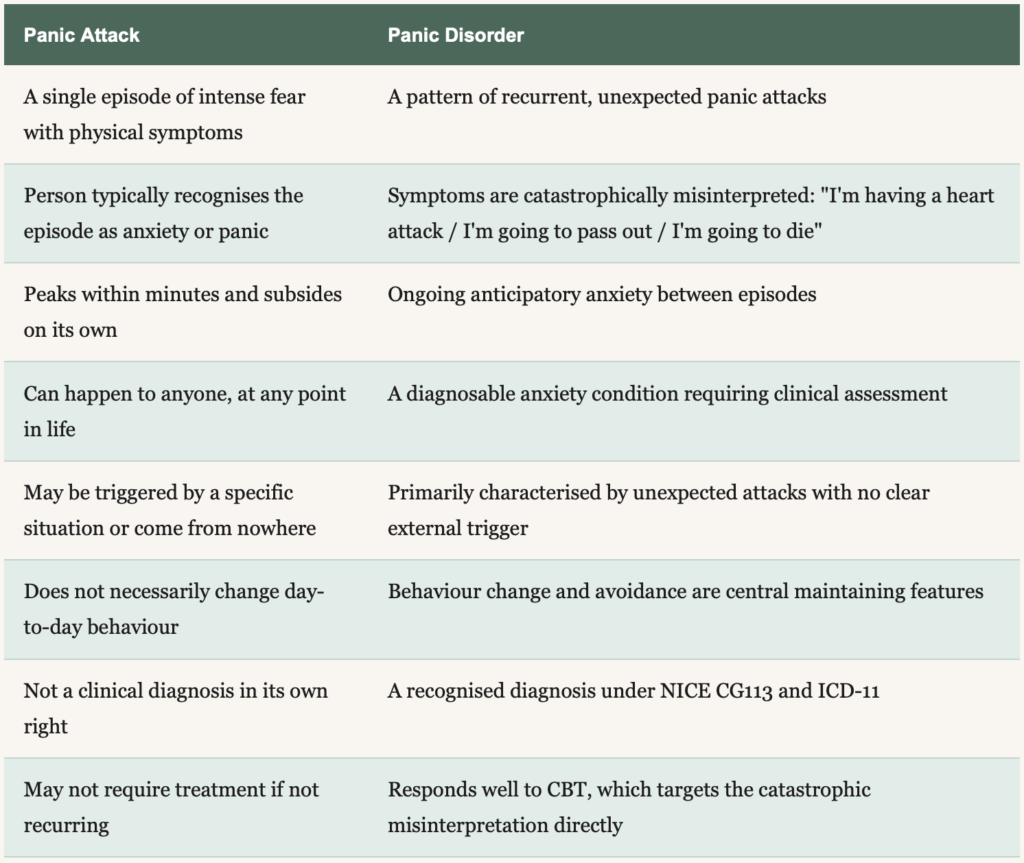
The key differences between a panic attack and panic disorder
The distinction comes down to pattern, context, and a clinically important difference in how the symptoms themselves are interpreted. One of the key things a therapist is looking for when assessing for panic disorder is catastrophic misinterpretation: whether the physical sensations of a panic attack are being read as signs of something medically dangerous or life-threatening, rather than recognised as anxiety.
In a panic attack without an underlying disorder, the person experiencing it typically knows, or comes to know, what is happening. It is frightening and overwhelming, but it is understood as panic or anxiety. In panic disorder, the same physical sensations, the racing heart, the breathlessness, the dizziness, are interpreted catastrophically: I am having a heart attack. I am going to pass out. I am going to die. That misinterpretation is not a symptom of severity. It is a diagnostic feature that shapes how the whole experience unfolds and why it escalates into a disorder rather than remaining an isolated event. It is also what CBT for panic disorder targets directly.

Not sure which type of support fits what you're experiencing? You can find out more about the support I offer.
When does a panic attack become panic disorder?
This is the question people most often ask, and it is the right one. A single panic attack, however terrifying, does not become panic disorder unless the aftermath creates a second problem: the fear of it happening again.
The clinical shift happens when you begin to live around the possibility of another attack. This might look like monitoring your body constantly for warning signs. It might look like avoiding the place, situation, or physical sensation that seemed to precede the first episode. It might look like seeking reassurance from doctors repeatedly about your physical symptoms, researching your symptoms online, or quietly reorganising your week so that you are never too far from somewhere you feel safe.
When that reorganisation becomes significant enough to restrict daily life, or when anticipatory anxiety is present between attacks, panic disorder is likely the more accurate description of what is happening. The threshold is not simply the number of attacks. It is what those attacks are doing to the shape of your life in between them.
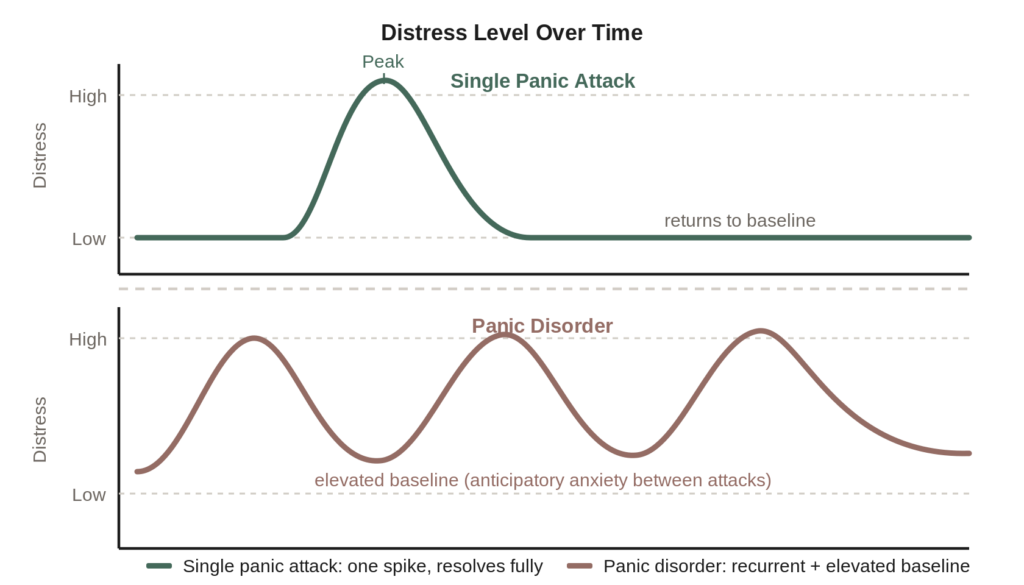
Illustrative representation based on clinical descriptions in NICE CG113 and the Royal College of Psychiatrists.
How does agoraphobia fit into panic disorder?
Agoraphobia is frequently misunderstood as a fear of open spaces. It is more accurately described as anxiety about situations in which escape might be difficult, or help unavailable, if a panic attack occurs. The NHS notes that it often develops alongside panic disorder as the avoidance behaviour that begins as a reasonable-seeming response to one situation gradually expands into others.
It might start with avoiding a specific Tube line. Then public transport generally. Then crowded shops. Then anywhere that involves queuing or waiting. For some people it eventually includes leaving the house. The original panic attack might have happened years ago. The avoidance it spawned has been quietly narrowing life ever since, in ways that can be hard to notice when the changes happen incrementally.
Not everyone with panic disorder develops agoraphobia, and agoraphobia can exist without a history of panic disorder. But the two are closely linked clinically. CBT for panic disorder addresses avoidance behaviour directly as a maintaining factor. Treating the panic without treating the avoidance leaves the architecture of the problem intact.
When is CBT right for you?
CBT is not always the right immediate response to a panic attack, and there is no value in seeking therapy before it is needed. If you have had one panic attack that resolved, you are not currently worried about having another, and it has not changed your behaviour in any meaningful way, watchful waiting is a reasonable and clinically supported first step.
CBT becomes the right choice when any of the following applies:
- You have had more than one unexpected panic attack and are worried about experiencing more.
- You are monitoring your body between attacks for signs that another one might be coming.
- You have started avoiding situations, places, physical sensations, or activities because of what they might trigger.
- Panic attacks are disrupting your work, relationships, or the way you spend your days.
- You have sought medical reassurance about your physical symptoms multiple times and the anxiety remains.
- The fear of having a panic attack is now more disruptive than the attacks themselves.
If you recognise yourself in that list, you are not overreacting. You are describing panic disorder, and panic disorder is something CBT was specifically designed to treat.
NICE guideline CG113 recommends CBT as the first-line psychological treatment for panic disorder in adults. The guideline specifies up to 12 to 15 hours of therapist contact for most presentations. Research underpinning the NICE recommendation consistently shows that CBT for panic disorder produces significant improvement in the majority of people who engage with it. It is not a last resort. It is the evidence-based starting point.
Related: CBT and ERP Therapy for OCD: What Sessions and Recovery Look Like | View Anxiety and Panic Services
What does CBT for panic disorder actually involve?
CBT for panic disorder is structured, time-limited, and built around a specific clinical model of what maintains panic. It is not general talking therapy. The focus is on the thoughts, physical sensations, and behaviours that keep the panic cycle running, and on changing each of them directly and systematically.
Psychoeducation: understanding the alarm system
The first stage involves understanding what is actually happening during a panic attack. The fight-or-flight response is your body doing precisely what it was designed to do: flooding your system with adrenaline, accelerating your heart rate and breathing, and preparing every muscle for action in response to perceived danger. The problem in panic disorder is that this response is being triggered by internal sensations, such as a slightly elevated heart rate or a wave of dizziness, rather than external threats. Understanding this changes how those sensations feel, because you understand what they are and, crucially, what they are not.
Identifying the maintaining cycle
Your therapist will help you map the specific cycle maintaining your panic: the trigger (internal or external), the physical sensations that follow, the catastrophic interpretation you apply to them, the anxiety spiral those interpretations produce, and the safety behaviours and avoidance that follow. That map is the basis of everything that comes next.
Cognitive restructuring
Unlike CBT for OCD, where engaging with thought content is deliberately avoided, CBT for panic disorder does address the interpretations being applied to physical sensations. Catastrophic misinterpretation, believing a racing heart means a heart attack, that dizziness means collapse, or that breathlessness means suffocation, is a central maintaining factor. Working through these interpretations, with evidence and direct experience rather than reassurance, reduces the threat value of the sensations themselves.
Interoceptive exposure
Interoceptive exposure is one of the most distinctive components of CBT for panic disorder. It involves deliberately inducing the physical sensations associated with panic in a controlled way: spinning in a chair to produce dizziness, running on the spot to elevate the heart rate, breathing through a narrow straw to create the sensation of breathlessness. The goal is to break the conditioned fear response to these sensations by demonstrating, repeatedly and directly, that elevated heart rate is not dangerous, dizziness is not collapse, and breathlessness is not suffocation. This requires a therapist with specific experience in panic-focused CBT.
Behavioural experiments and dropping safety behaviours
Any situation or place that has become associated with panic and is now avoided is worked through systematically in a gradual way. Safety behaviours, the things you do to feel safer during a potential attack, such as carrying water, sitting near exits, keeping your phone visible, or only going out with a specific person, are addressed directly. These behaviours feel protective but maintain the belief that the situation is genuinely dangerous without them. Dropping them, with support, is how that belief changes.

What recovery from panic disorder looks like
Recovery does not mean your nervous system becomes incapable of producing anxiety or that you will never feel the physical sensations associated with panic. It means the relationship with those experiences changes fundamentally. An elevated heart rate becomes information rather than an alarm. You can be in a crowded place, on the Tube, or in a queue, notice the old sensation, and not trigger the old spiral. The gap between sensation and catastrophe widens until it is too wide to bridge automatically.
In practical terms, recovery from panic disorder looks like getting back the places, situations, and activities that avoidance had quietly removed. It looks like making decisions based on what you actually want to do, not on what feels safest. It looks like understanding what your nervous system is doing when it produces those sensations, and meeting it with accurate information rather than escalating fear.
The Royal College of Psychiatrists notes that most people who engage with CBT for panic disorder experience significant improvement. The research base underpinning NICE CG113supports this consistently. Panic disorder is one of the more treatment-responsive anxiety conditions, and the gains made in CBT tend to be durable. That does not mean it resolves without effort. It means the effort has a reliably high chance of working.
Anxiety UK notes that panic disorder, when left untreated, tends to become more restrictive over time as avoidance expands. Seeking treatment before avoidance becomes deeply entrenched typically produces faster and more durable results. The longer avoidance is in place, the more systematic the exposure work needs to be, but the evidence base for CBT holds across presentations of varying severity and duration.
If any of this sounds familiar and you're wondering whether CBT might help, I offer a free 15-minute consultation — no pressure, just a conversation.
Frequently Asked Questions
ABOUT THE AUTHOR
Who writes this?

Evelynne R. Scott-McFarlane
BABCP ACCREDITED CBT THERAPIST
I'm a BABCP accredited CBT therapist specialising in anxiety - OCD, health anxiety, and panic disorder. I trained at King's College London and work online with clients across London and the UK.
I write these articles because good information is hard to find. Most mental health content online is either too vague to be useful or too clinical to be readable. I'm trying to do something different

![]()
